Abstract
Nanotechnology contributes towards a more effective eradication of pathogens that have emerged in hospitals, veterinary clinics, and food processing plants and that are resistant to traditional drugs or disinfectants. Since new methods of pathogens eradication must be invented and implemented, nanotechnology seems to have become the response to that acute need. A remarkable achievement in this field of science was the creation of self-disinfecting surfaces that base on advanced oxidation processes (AOPs). Thus, the phenomenon of photocatalysis was practically applied. Among the AOPs that have been most studied in respect of their ability to eradicate viruses, prions, bacteria, yeasts, and molds, there are the processes of TiO2/UV and ZnO/UV. Titanium dioxide (TiO2) and zinc oxide (ZnO) act as photocatalysts, after they have been powdered to nanoparticles. Ultraviolet (UV) radiation is an agent that determines their excitation. Methods using photocatalytic properties of nanosized TiO2 and ZnO prove to be highly efficient in inactivation of infectious agents. Therefore, they are being applied on a growing scale. AOP-based disinfection is regarded as a very promising tool that might help overcome problems in food hygiene and public health protection. The susceptibility of infectious agents to photocatalylic processes can be generally arranged in the following order: viruses > prions > Gram-negative bacteria > Gram-positive bacteria > yeasts > molds.
Similar content being viewed by others
Review
Introduction
Some metal oxides powdered to nanoparticles (NPs) (1 < φ ≤ 100 nm) have been attracting much interest among scientists representing various fields of science. The main reason for this ever growing interest presents photocatalytic properties that those compounds exhibit. Photocatalytic properties of titanium dioxide (TiO2) were first reported in the 1970s [1] and later confirmed in a number of experiments [2–5]. At the end of the twentieth century, the studies that were going on in various research centers discovered that also other metal oxides, e.g., zinc oxide (ZnO) [6–10], after they have been powdered to the NP form, exhibit formerly undisplayed photocatalytic properties. Due to those newly discovered characteristics, TiO2 and ZnO in the NP form have found many new applications, e.g., as ingredients of photocatalytic layers covering various work surfaces [11]. The so-coated surfaces gain self-disinfecting and self-cleaning abilities [12, 13]. It is a result of advanced oxidation processes (AOPs) initiated by the ultraviolet (UV) radiation [14]. On surfaces coated by a thin film of photocatalyst, the inactivation of infectious agents [15, 16] and the mineralization of organic matter [17, 18] take place. Due to their virucidal [19, 20], bactericidal [21, 22] and fungicidal [23, 24] properties, photocatalytic layers are increasingly applied to coat surfaces in miscellaneous premises, such as farms, abattoirs, production halls, hospitals, and laboratories. The usefulness of photocatalysis has also been proven in water treatment [25], purification of drinking water [26], and air disinfection [27]. The researchers presume that the introduction of photocatalytic surfaces in the food industry, animal production, and health-care facilities will also be beneficial, as it will help prevent food poisonings and food contaminations, contribute towards the animal welfare, and improve the efficiency of pathogen eradication [28–30].
Photocatalytic Properties of Titanium and Zinc Oxides
The discovery in the second half of the twentieth century that nanosized titanium dioxide (nano-TiO2) exhibits catalytic properties if exposed to UV radiation evoked a great interest in this substance [1] that has been growing ever since [14, 31]. The photocatalytic properties of semiconductors, to which nanosized metal oxides, such as TiO2 and ZnO, belong, result from their specific energetic structure. Their low-energy valence band (VB) is filled with electrons, and their high-energy conduction band (CB) is electron free. The energy difference (ΔE) between those bands, defined as band gap, equals the amount of energy necessary to excite an electron from VB to CB. In case of three polymorphic TiO2 forms, i.e., brookite, rutile, and anatase, as well as for ZnO, the width of the energy gap amounts to 2.96, 3.02, 3.20, and 3.37 eV, respectively. It is the equivalent of the electromagnetic radiation photon energy with a wavelength of λ < 400 nm. The photocatalytic properties of TiO2 and ZnO in their NP form are applied in a number of biological experiments, in which the UV radiation is used with the purpose to excite the photocatalysts. The UV radiation is commonly applied in its near-ultraviolet range (UV-A, λ = 315–400 nm) [32–37].
The result of the semiconducting metal oxides irradiation is the excitation of an electron (e−) from VB to CB, whereby a positively charged electron hole (h+) emerges. Therefore, a specific “hole-electron” pair (h+ + e−), called exciton, is generated [38, 39] (Fig. 1).
Mechanism of reactive oxygen species (ROS) generation on the surface of nanoparticles of titanium or zinc oxides (a) and the effects of ROS on infectious agents (b). On the surface of TiO2 and ZnO nanoparticles, exposed to UV radiation, ROS (•O2 −, •OH, and H2O2) are formed (a). ROS have the ability to inactivate infectious agents susceptibility of which to oxidative damages can be arranged in the following order: viruses > prions > Gram(−) bacteria > Gram(+) bacteria > yeasts > molds (b). Subsequently, organic matter and dead microbial cells are oxidized by ROS to CO2 and H2O (b)
The electron holes (h+) induce the oxidation processes while electrons (e−) condition the reduction processes. The electron holes (h+) react with water molecules (H2O) or hydroxide ions (OH−), forming hydrogen peroxide molecules (H2O2) or hydroxyl radicals (•OH). Electrons (e−) react with molecular oxygen (O2), forming superoxide anion radicals (•O2 −). Therefore, various forms of reactive oxygen species (ROS) are created: H2O2, •OH, and •O2 − [38–40] (Fig. 1).
ROS emerging on the photocatalytic surfaces first inactivate infectious agents such as viruses, prions, bacteria, yeasts, and molds. Then, ROS oxidize the dead microbial cells [23, 24, 41], along with organic matter [18, 42], to CO2 and H2O. Due to photocatalytic properties, TiO2 and ZnO are applied, after powdering to NPs, in AOPs- and UV-radiation-based methods of pathogens inactivation and organic pollutants decomposition [43]. The susceptibility of infectious agents to photocatalylic processes may by miscellaneously arranged, depending upon particular studies presented by various authors. The most representative seems to be in the following order: viruses > prions > Gram-negative bacteria > Gram-positive bacteria > yeasts > molds (Fig. 1).
Antiviral and Antiprion Activity of Nanosized Titanium Dioxide
Viruses Inactivation
There are studies proving that the TiO2/UV process where titanium dioxide (TiO2), after it has been powdered to nanoparticles, performs as photocatalyst, and ultraviolet (UV) radiation is an agent generating reactive oxygen species, is an effective tool in the eradication of many viruses from a number of taxonomy groups (according to the Baltimore system of virus classification) [44, 45]. Among viruses inactivated by the TiO2/UV process, there are: icosahedral enveloped viruses from the dsDNA group, e.g., herpes simplex virus type 1 (HSV-1) [42, 46], and from the dsDNA-RT group, e.g., hepatitis B virus (HBV) [47]; icosahedral non-enveloped viruses from the dsRNA group, e.g., rotavirus A (RV-A) [48], and from the (+)ssRNA group, e.g., poliovirus (PV) [49]; helical enveloped viruses from the (−)ssRNA group, e.g., avian influenza H5N2 virus (A/H5N2) [43]; as well as icosahedral phages of Escherichia coli, such as MS2 from the (+)ssRNA group [35, 50, 51] and T4 from the dsDNA group [52, 53]. In the past, air-borne virus diseases appeared to pose a serious health risk for large human populations. As an example, severe acute respiratory syndrome (SARS) can be quoted. It was detected in China in 2003, for the first time. Another example is the influenza epidemic that spread over the whole world in 2009, growing to nearly pandemic dimensions. Nonspecific character of AOPs gives rise to assume that the TiO2/UV process could efficiently reduce the dissemination of many viruses, e.g., measles, mumps, rubella, or smallpox. Some authors, like Han et al. [54], believe the TiO2/UV process can be an efficient tool to reduce the dissemination of the SARS virus, a helical enveloped virus from the (+)ssRNA group. Nakano et al. [55] showed that on the surface covered by a thin layer of nano-TiO2, a complete inactivation of influenza virus took place within a short period (approximately 30 min) of the TiO2/UV process. Those results have also been confirmed in the studies of other authors [56]. Despite the common opinion of the relatively high virus susceptibility to AOPs (Fig. 1), Josset et al. [57] and Zhao et al. [58] suggest a higher (compared to bacteria) resistance of viruses to photocatalytic processes.
The virus inactivation mechanism by AOPs is still insufficiently examined [59]. Kashige et al. [60] suggest the TiO2/UV-based inactivation of the phage PL-1 that infects Lactobacillus casei should be attributed mainly to the damages of capsid proteins inflicted by hydroxyl radicals and superoxide anion radicals. As the authors report, the fragmentation of the viral nucleic acid follows. The same opinion with respect to the MS2 phage infecting E. coli represents Kim et al. [61] as well as Sjogren and Sierka [62]. According to Liga et al. [63, 64], non-enveloped viruses are more prone to the oxidizing activity of hydroxyl radicals than enveloped viruses. Their nucleic material is separated from the external environment only by a thin layer of capsid. In enveloped viruses, the nucleocapsid, also called virion, is surrounded by a plasma membrane that protects the viruses from external factors. This envelope is formed of virus-produced glycoprotein spikes and of a phospholipid bilayer derived from the host cell and composed by phosphatidylethanolamine (PE). In all herpesviruses, there is a tegument, a protein cluster, which is located between the envelope and nucleocapsid [46]. Xu et al. [59] report that the differences between the enveloped and non-enveloped viruses in their susceptibility to photocatalytic processes result from the number of layers, hence the difference in the overall thickness, separating the virus nucleic material from the external environment, rather than from the various susceptibilities of the particular layers that surround the nucleic material (Fig. 2).
Not all authors share, however, the above outlined conclusions. Nakano et al. [65] report that the non-enveloped viruses exhibit greater resistance to the destructive activity of the TiO2/UV process. In their experiments, they examined the susceptibility of two viruses: an influenza virus (IFV), a representative of the enveloped viruses group, and a feline calicivirus (FCV) from the non-enveloped viruses group. Both viruses were inactivated in a time-dependent manner. It took for the inactivation of FCV to fall below the detection limit as much as twice the time as it was needed in case of IFV. The authors suggest those differences are attributed to the viral envelope. The products of peroxidation of the envelope membrane phospholipids promote the oxidative damages to capsid proteins. As a consequence, the damages to nucleic acid, hence the virus inactivation, occur faster.
Prions Inactivation
Hydroxyl radicals formed during the TiO2/UV process inactivate also protein infectious agents, so-called prions. Prions belong to the group of pathogens that exhibit a fairly high resistance to conventional disinfection methods. Paspaltsis et al. [66, 67] observed in vitro the full decomposition of the scrapie prion protein (PrPSc), a protein causing one of the several transmissible spongiform encephalopathies (TSEs), after 60 min of UV-A irradiation in the presence of 0.8 % colloidal nano-TiO2. The researchers also reported that the decomposition of the cellular prion protein (PrPC), a protein not inducing any of the TSEs, took place already after 30 min of the TiO2/UV process. A greater resistance of PrPSc to oxidative activity of ROS is attributed to alleged differences in the protein secondary structure, a reason for the protein’s different physicochemical properties. Paspaltsis et al. [66, 67] stress that the dimensional structure of PrPSc still remains hypothetical. Due to its insolubility in water, it is impossible, though, to examine PrPSc using nuclear magnetic resonance (NMR) spectroscopy. Prion transmission, hence prion-induced diseases, constitutes a serious risk for the health of people and animals alike. The main source of infection is the contamination of surgeon tools by prions. The implementation of the TiO2/UV-based disinfection of medical tools and devices in the human and veterinary medicine might help reduce the number of TSEs infections on the iatrogenic pathway.
Antibacterial Activity of Nanosized Titanium and Zinc Oxides
Contemporary human and veterinary medicine have found measures to prevent and heal many bacterial diseases, using traditional methods, such as vaccination and antibiotic therapies. Nonetheless, numerous microorganisms present in clinical and non-clinical environments have recently become much more resistant to drugs [68]. Currently, the main problem in hospitals and veterinary clinics is the presence and infestation of highly virulent and antibiotic-resistant pathogens. Among them, there are Gram(−) bacteria, e.g., carbapenem-resistant Acinetobacter baumanii (CRAB) [69], carbapenem-resistant Klebsiella pneumonia (CRKP) [70], carbapenem-resistant Pseudomonas aeruginosa (CRPA) [71], as well as Gram(+) bacteria, e.g., vancomycin-resistant enterococci (VRE) [72], methicillin-resistant Staphylococcus aureus (MRSA) [73], vancomycin-resistant S. aureus (VRSA) [74], methicillin-resistant Staphylococcus epidermidis (MRSE) [73], or penicillin-resistant Streptococcus pneumoniae (PRSP) [75]. Thus, the search for effective methods of pathogen eradication presents a crucial challenge for many research centers in the world [21, 22, 76]. One of the latest achievements in this field has been the application of photocatalysis [77].
Titanium Dioxide
Nano-TiO2 exhibits not only virucidal properties. The TiO2/UV process is a tool for an efficient bacteria eradication, too [77–83]. Its antibacterial activity depends upon such factors as light intensity [2], concentration and diameter of photocatalyst particles [10, 84], temperature of environment [3], chemical composition of the base [85, 86], and sensitivity of microorganism species [87, 88]. According to Ferin and Oberdörster [89] as well as Hwang et al. [90], the highest photocatalytic activity, hence the strongest bactericidal properties are shown by two polymorphic forms of nano-TiO2, anatase, and rutile, combined in the proportion 80 and 20 %, respectively. This composition is widely used in experiments with bactericidal properties of nano-TiO2 and is commonly known under the trade name P-25 [91]. Some literature reports that both forms (anatase and rutile) are equally harmful to bacteria [10]. However, most authors report that anatase shows stronger catalytic properties than rutile [92]. Various studies examined the optimal concentration of P-25 in aqueous solutions for the purpose of bacteria eradication. Liou and Chang [93] as well as Pigeot-Rémy et al. [94] prove that, irrespectively of the initial density of E. coli cells (102–108 CFU mL−1), the highest bacteria inactivation rate was observed at 0.1 % P-25. Other authors concentrated on the influence of the diameter of nano-TiO2 particles on its bactericidal properties. Salih and Pillay [95], as well as many other scientists [96, 97], came to the conclusion that nano-TiO2 with φ < 20 nm has stronger bactericidal properties than its less powdered form. It can be attributed to the fact that particles with φ < 20 nm are able to penetrate the damaged cell envelope (cell wall and plasma membrane) and infiltrate the cytosol while particles with φ = 20–80 nm are not able to overcome the barrier of a cell envelope. The nano-TiO2 particles’ antibacterial activity increases as their size decreases (surface-area-to-volume ratio). The smaller the NP size, the bigger the surface area of the nano-TiO2 particles, hence the number of ROS. Other studies point out that environmental factors affect the efficiency of the TiO2/UV process. Tong et al. [86] indicate that various factors, including organic pollutants, may cause a decrease of bacteria inactivation rate, even by 40 %. Results of other experiments suggest the underlying factor to weaken the nano-TiO2 photocatalytic effect might also be the high density of microorganism cells (in excess of 108 CFU mL−1) [2, 85, 98].
The studies on the susceptibility of bacteria to the TiO2/UV process date back to 1985 when Matsunaga et al. [4] for the first time reported that a 120-min exposition of water polluted by E. coli and Lactobacillus acidophilus to the UV-A radiation resulted in an almost complete destruction of the bacteria. This experiment used photocatalytic properties of the nanosized titanium dioxide loaded by platinum (nano-TiO2/Pt). The NPs’ addition of some chemical elements, both metals (e.g., Ag, Au, and Pt) and non-metals (e.g., C, N, and P), as well as their oxides (e.g., WO3 and CrO3), results in the broadening of the electromagnetic radiation spectrum capable of exciting electrons in a semiconductor, e.g., nano-TiO2, and thereby enhances its effectiveness as a photocatalyst [5, 99]. In the inactivation of bacteria by the TiO2/UV process, ROS plays a crucial role. The strongest bactericidal activity among the ROS is attributed to hydroxyl radicals [14, 18, 36, 38, 100]. Cho et al. [101] claim there is a linear correlation between the E. coli inactivation rate and the hydroxyl radical concentration in bacteria cells. Bekbölet and Araz [102] as well as Salih [103] maintain that high oxidation potential and nonspecific reactivity of hydroxyl radicals are the main factors of their bactericidal properties. Hydroxyl radicals (•OH) are short living, particularly unstable and react rapidly with most biological molecules [40]. They can penetrate the cell wall, oxidize membrane fatty acids, induce lipid peroxidation, oxidize proteins, and damage DNA. Proteins are affected by tyrosine hydroxylation, oxidation of methionine or cysteine, as well as by the carbonyl group formation on side-chain amino acids [104, 105]. Similar effects are induced by hydrogen peroxide molecules (H2O2) [36, 106, 107] (Fig. 3).
Bacteria cell structures most easily damaged by reactive oxygen species (ROS). Among the bacteria cell structures, cell envelope (cell wall and plasma membrane) as well as nucleoid are most affected by ROS-induced damages. Hydroxyl radicals (•OH) and hydrogen peroxide molecules (H2O2) have the ability to penetrate the bacteria cell envelope, whereas superoxide anion radicals (•O2 −) do not exhibit such ability
During the oxidation of the bacteria cell envelope phospholipids, carbonyl compounds such as aldehydes, ketones, and carboxylic acids are formed. Some of them exhibit properties that are potentially toxic to bacteria [16, 108]. Liu et al. [105], as well as other authors [109, 110], observed at the model of E. coli that various layers of the bacteria cell envelope are characterized by a different susceptibilities to hydroxyl radicals generated as a result of photocatalytic processes, e.g., the TiO2/UV process. According to those authors, the highest resistance was shown by peptidoglycan (PG), also called murein. In Gram-positive bacteria, the PG provides for an efficient physical barrier that prevents from the entry of molecules into the cell. Much more susceptible to oxidative damages was PE that builds a phospholipid bilayer of plasma membrane, while lipopolysaccharides (LPS), present exclusively in outer membrane of Gram-negative bacteria cell wall, submitted particularly easy to the oxidative damages. Porins going across the outer membrane facilitate small molecules to enter the cells. In bacteria exposed to the TiO2/UV process, significant morphological changes in the cell structure were observed, using the scanning electron microscopy (SEM), transmission electron microscopy (TEM), and atomic force microscopy (AFM) [111, 112]. Various cell damages were noticeable, e.g., plasmolysis, intracellular vacuoles ghost, cell debris, and nucleoid condensation [113, 114]. In some cases, a separation of the plasma membrane from the PG layer occurred. As a general rule, the bacteria inactivation progressed with no visible PG degradation, neither with Gram-negative nor with Gram-positive bacteria [115]. Hydroxyl radicals (•OH), generated during the TiO2/UV process, infiltrate the cell envelope, subsequently disrupting nucleic acids. They destroy phosphodiester linkages, induce the formation of pyrimidine dimers [32, 100, 116, 117], or lead to a complete oxidation of purine and pyrimidine bases to CO2, H2O, and NH3 [17, 18]. Hydroxyl radicals can also damage the DNA of bacterial plasmid [118] and induce the dimerization of coenzyme A (CoA) particles [119]. The CoA is the intracellular carrier of acyl groups and electrons. Its depletion disrupts the process of oxidative pyruvate decarboxylation and the Krebs cycle, both important stages of glucose catabolism. The increase in the concentration of the dimeric CoA inhibits the cell respiration. Imlay et al. [120], similarly Ndounla et al. [121], emphasize that the formation of bactericidal hydroxyl radicals does not occur exclusively as a consequence of nano-TiO2 excitation by UV radiation. As they report, a simultaneous process is the Fenton reaction. There, the formation of hydroxyl radicals (•OH) is actively enhanced by Fe2+ ions and hydrogen peroxide molecules (H2O2) (see Eq. 1).
Superoxide anion radicals (•O2 −) cannot penetrate the cell envelope since they are negatively charged. However, contrary to hydroxyl radicals, they show a relatively long living period [36] (Fig. 3).
Bacteria, similar to cells of eukaryotic organisms, have also developed their own antioxidant enzyme systems, i.e., mechanisms protecting them from ROS. The principal defense mode is a system of three enzymes that are responsible for detoxification of ROS. These are: superoxide dismutase (SOD; EC 1.15.1.1), a protein catalyzing the disproportionation reaction of two superoxide anion radical particles to hydrogen peroxide and molecular oxygen and catalase (CAT; EC 1.11.1.6) and glutathione peroxidase (GPX; EC 1.11.1.9), enzymes decomposing hydrogen peroxide into water and molecular oxygen [122, 123]. The crucial role in limiting the negative effects of oxidative stress plays also as antioxidants such as lipoic acid (LA) and ubiquinone (CoQ10). LA is considered to be an important endogenous free radical scavenger as it neutralizes free radicals in lipid and aqueous domains alike. CoQ10 performs also as an energy carrier. Kim et al. [124] and Ojima et al. [125] confirmed in their experiments with E. coli that in case the ROS concentration is too high for the defense systems to repair, numerous oxidative damages of the nucleoid and cell envelope phospholipids domain occur. The products of polyunsaturated fatty acids (PUFAs) peroxidation, such as malondialdehyde (MDA), can form adducts with nucleic acids and proteins thus, leading to alterations in their functioning. The DNA damages result in various mutations, while the protein injuries cause enzymes inhibition, denaturation and protein degradation. As those alterations become excessive, they may eventually lead to the cell death. Simon-Deckers et al. [10] studied other Gram-negative bacteria, Cupriavidus metallidurans, and stated that the cell death is, on the one part, a result of the amount of ROS and the extent of the damages caused by them; and, on the other part, a result of the ability to keep the cell envelope integrity by the intracellular repair systems.
Sunada et al. [126] represent the opinion that the bacteria inactivation during the TiO2/UV process takes place in three steps. At first, oxidative damage of the outer membrane occurs, causing merely insignificant impairment to bacteria viability. Thereafter, a DNA injury, the lowering of CoA level, increased permeability of the plasma membrane and the leakage of the intracellular components follow. Finally, the microorganisms die.
The differentiation in the bacteria susceptibility to the TiO2/UV process results from two factors: various structure of the cell wall (its complexity and thickness) and different susceptibilities of the cell wall compounds to oxidative damages. Bactericidal effects that the TiO2/UV process has on many microorganisms have been confirmed. Moderate resistance against oxidative damages was exhibited by the Gram-negative bacteria, e.g., E. coli [2, 5, 33, 34, 79, 86, 98, 99, 105, 119, 124, 127–133], K. pneumoniae [134], Salmonella Enteritidis [37, 135], Salmonella Typhimurium [127], Serratia marcescens [136], Shigella flexnerii [15, 127], Legionella pneumophila [137], A. baumannii [15, 128, 136], P. aeruginosa [34, 37, 77, 78, 129, 138, 139], and Vibrio cholerae [127]. Gram-negative bacteria have a fairly thin cell wall (2–10 nm) which is formed of two phospholipid bilayers (outer membrane and plasma membrane), separated by periplasmic space in which two to three PG layers are immersed. Murein is a net of long, unbranched chains formed of particles of n-acetylglucosamine (GlcNAc) and n-acetylmuramic acid (MurNAc) that are alternately arranged and linked by β-1,4-glicosidic bond. The chains are bound by transversal (horizontal and vertical) oligopeptide bridges. Unlike the plasma membrane, which is formed almost exclusively of PE, the outer membrane consists of two asymmetrically placed lipid layers. The inner layer is formed of PE, and the outer layer of LPS that in pathogens play the role of endotoxins and are a significant pathogenic agent [105, 108, 110] (Fig. 4).
Susceptibility ( ) of Gram-negative bacteria cell envelope compounds to damages induced by hydroxyl radicals (•OH). Susceptibility of the various compounds of the Gram(−) bacteria cell envelope (cell wall and plasma membrane) to oxidative damages presents the following order: lipopolysaccharides > phospholipids > peptidoglycan
) of Gram-negative bacteria cell envelope compounds to damages induced by hydroxyl radicals (•OH). Susceptibility of the various compounds of the Gram(−) bacteria cell envelope (cell wall and plasma membrane) to oxidative damages presents the following order: lipopolysaccharides > phospholipids > peptidoglycan
A greater resistance to the destructive properties of ROS show Gram-positive bacteria species, e.g., S. aureus [15, 34, 76, 129, 140], Bacillus anthracis [141–144], Bacillus cereus [145], Bacillus pumilis [146], Bacillus subtilis [33, 141], L. acidophilus [4, 147], Lactobacillus helveticus [130], Clostridium perfringens [148], Enterococcus faecalis [149], Enterococcus faecium [34], and Listeria monocytogenes [78, 136, 150, 151]. Gram-positive bacteria have a relatively thick cell wall (20–80 nm). Their plasma membrane is formed similarly as in Gram-negative bacteria and is surrounded by around 40 layers of PG. Long, polymeric, and sticking over the surface of cell wall chains of teichoic acids pass across murein. Lipoteichoic acid (LTA) is rooted in plasma membrane whereas teichoic acid (TA) is bound to polysaccharide murein chains (more precisely, to the groups of MurNAc) [108, 110] (Fig. 5).
Susceptibility ( ) of Gram-positive bacteria cell envelope compounds to damages induced by hydroxyl radicals (•OH). Susceptibility of the various compounds of the Gram(+) bacteria cell envelope (cell wall and plasma membrane) to oxidative damages presents the following order: phospholipids > peptidoglycan
) of Gram-positive bacteria cell envelope compounds to damages induced by hydroxyl radicals (•OH). Susceptibility of the various compounds of the Gram(+) bacteria cell envelope (cell wall and plasma membrane) to oxidative damages presents the following order: phospholipids > peptidoglycan
As Markowska-Szczupak et al. [152] report, the bacterial susceptibility to the TiO2/UV process can be ordered as follows: E. coli > Gram-negative bacteria (other than E. coli) > Gram-positive bacteria (other than Enterococcus sp.) > Enterococcus sp. (Fig. 1). This sequence is confirmed also by Kühn et al. [34] who arranged the inactivation effectiveness of four bacteria species on a surface covered by a thin layer of nano-TiO2 and exposed to UV-A radiation during 60 min as follows: E. coli > P. aeruginosa > S. aureus > E. faecium. The experiments conducted by Hitkova et al. [153] confirm that Gram-negative bacteria are more susceptible to the photocatalytic inactivation than Gram-positive bacteria. The entire reduction of E. coli and P. aeruginosa, two Gram-negative bacteria representatives, was achieved within 15 and 25 min, respectively, while it took 35 min to completely inactivate S. aureus, a Gram-positive bacteria species. A great number of studies confirm the above outlined susceptibility sequence [62, 78, 81, 101, 154–160]. There are, however, authors who report the opposite order [4, 161–163]. According to them, the Gram-negative bacteria are more resistant to oxidative damages. Nakano et al. [65] examined the period needed to entirely inactivate S. aureus, a Gram-positive bacteria. It appeared to be four times shorter than that needed to destroy E. coli and S. marcescens, two Gram-negative bacteria species. Kubacka et al. [164] and Wolfrum et al. [24] reported there was no difference in sensitivity between the Gram-negative and Gram-positive bacteria.
Numerous studies confirm the high effectiveness of TiO2/UV process in eradication of methicillin-resistant S. aureus (MRSA) [73, 165, 166] and of UV-resistant Enterobacter cloacae [167]. Hydroxyl radicals that are formed during the TiO2/UV process have high oxidation potential, and they can also eradicate spores of B. anthracis and B. cereus [141–143].
Zinc Oxide
The nanosized zinc oxide (nano-ZnO) exhibits strong bactericidal properties when exposed to the UV radiation. Therefore, the ZnO/UV process presents another example of a tool that provides for an efficient bacteria eradication. The inactivation is effective for many species of Gram-negative (e.g., E. coli, L. monocytogenes, S. Enteritidis) and Gram-positive bacteria (e.g., B. subtilis, S. aureus, Streptococcus pyogenes, E. fecalis) [6–9, 78, 130, 168–171]. According to some authors [7, 8, 172, 173], bactericidal effects of nano-ZnO are directly and inversely proportional to the concentration and diameter of its particles, respectively. Having used the confocal laser scanning microscopy (CLSM), Raghupathi et al. [172] concluded that the accumulation of nano-ZnO in the cytoplasm or on the outer membrane might be involved in the antibacterial activity of nano-ZnO. Yamamoto [8] and Zhang et al. [9] emphasized that in the inactivation of bacteria by the ZnO/UV process, the crucial role played hydroxyl radicals and hydrogen peroxide molecules with their ability to infiltrate through the cell wall. The studies of Azam et al. [78] as well as Liu and Yang [130] showed that PE, the main component of the cell wall of Gram-negative bacteria, was much easier to penetrate by hydroxyl radicals and much more susceptible to oxidative damages than murein, the main component of the cell wall of Gram-positive bacteria. Thus, the cell wall of E. coli (Gram-negative bacteria) was easier to penetrate and damage by hydroxyl radicals and hydrogen peroxide molecules than the cell wall of S. aureus (Gram-positive bacteria) [6, 9, 78, 130]. In their experiments with Campylobacter jejuni, a Gram-negative bacteria, Xie et al. [174] observed that this very common food-borne pathogen was very sensitive to the ZnO/UV process. The overall growth impairment rate appears, therefore, clearly higher in case of Gram-negative bacteria. This conclusion was, however, not confirmed by Jain et al. [175] and Siddique at al. [173] who reported that nano-ZnO stronger restricts the growth of Gram(+) bacteria than Gram(−) bacteria.
Gordon et al. [168] examined the bacteria inactivation rate by superoxide anion radicals. According to them, negatively charged superoxide anion radicals did not infiltrate through the strongly negatively charged cell wall of E. coli as easily as through S. aureus cell wall which is formed mainly of PG, hence exhibits a lower density of the negative charge. This characteristic explains, as the authors say, the higher susceptibility of Gram(+) bacteria to superoxide anion radicals than that of Gram(−) bacteria.
As a matter of fact, the results of a great majority of experiments prove a higher susceptibility of Gram-negative bacteria (e.g. E. coli) to the ZnO/UV process than that of Gram-positive bacteria (e.g. S. aureus) [6, 9, 78, 130]. Such a difference in susceptibility is attributed to the different chemical composition and structure of the bacteria cell wall. Gram(−) bacteria have a much thinner cell wall compared to Gram(+) bacteria, and the content of PG, a compound relatively resistant to oxidative damages, in their cell wall is quite low.
Antifungal Activity of Nanosized Titanium and Zinc Oxides
Fungi play an important role in our everyday life. For instance, they influence the quality of the air in rooms. Allergies, asthma, or respiratory tract infections are just some of a great number of ailments conditioned by the presence of fungi in closed areas. Pollutions in buildings are often a factor inducing the so-called sick building syndrome [176]. Many researchers believe that AOPs taking place on surfaces covered by a thin layer of photocatalyst, such as nano-TiO2 or nano-ZnO, might be a tool to effectively restrict the dissemination of yeasts and molds, just as it is the case with viruses and bacteria harmful to humans and animals [4, 24, 80–83, 142].
Yeasts Inactivation
Pioneering studies evaluating the effectiveness of the TiO2/UV process in eradication of yeasts were conducted by Matsunga et al. [4] in 1985. They proved that the number of inactivated in vitro cells of Saccharomyces cerevisiae after 240 min of UV-A irradiation increased from 72 % to nearly 98 % as a result of application of 0.5 % colloidal nano-TiO2. Thabet et al. [177] reported there was no presence of nano-TiO2 particles in S. cerevisiae cells despite a long exposition of the pathogen to the TiO2/UV process, even though of the ROS concentration in cytosol increased. Those results suggest the damages in the cell wall and in the plasma membrane were merely insignificant. Fungicidal properties of nano-TiO2 have been also confirmed at the example of another representative of yeasts, Candida albicans [23, 80–82, 178, 179]. The growth of this pathogen was strongly impaired also in the presence of nano-ZnO [180–183]. According to Gondal et al. [181], the minimal inhibitory concentration (MIC) of nano-ZnO against C. albicans is 2.5 mg mL−1, a value nearly ten times higher than in case of bacteria. In both yeasts species, S. cerevisiae and C. albicans, vegetative forms exhibited a significantly lower resistance to AOPs compared to spores [80]. Lipovsky et al. [184] attribute the key role in the pathogen cells inactivation to ROS, particularly to hydroxyl radicals as agents that induce the cell envelope damages. Results of numerous studies have shown a lower susceptibility of yeasts to photocatalytic processes in comparison to bacteria [80–83, 87] (Fig. 1). Those findings have also been confirmed by the examination of their cell wall morphology, using the TEM and the X-ray diffraction (XRD) [183]. This reaction is attributed to the differences in the cell wall composition between those microorganisms [185]. Insofar the bacteria cell wall contains PG, a compound that is highly resistant to oxidative damages [105, 108, 110], the fungi cell wall contains instead a compound called chitin, which is even more resistant to the oxidative ROS activity [23]. Chitin is an unbranched polysaccharide formed of 100–160 groups of GlcNAc, linked by β-1,4-glycosidic bonds. In yeasts, this polysaccharide is present in deeper layers of the cell wall and amounts to only 1–3 % of its dry matter. The main component of the yeast cell wall is polysaccharides composed of d-glucose monomers, called glucans. In respect of their resistance to hydroxyl radicals, glucans only slightly lag behind chitin. In yeasts, mainly β-glucans are represented. A moderately branched β-1,3-glucan prevails, accompanied by much a more branched, less present β-1,6-glucan. The external layer of the yeasts cell wall is formed predominantly from mannoproteins, fairly susceptible to oxidative damages protein-sugar compounds, constituting around 40 % of cell wall dry matter. Plasma membrane formed mainly from PE and contiguous with cytosol shows the greatest susceptibility to oxidative injuries [186, 187] (Fig. 6).
Molds Inactivation
Recent studies prove that nanosized metal oxides, such as nano-TiO2 or nano-ZnO, can be applied to inactivate many species of molds (filamentous fungi), e.g., Fusarium oxysporum [83, 188], Aspergillus niger [81, 82, 181, 189], and Penicillium expansum [190, 191].
Chen et al. [192] reported that molds exhibit a lower resistance to the TiO2/UV process than viruses, bacteria, or even yeasts (Fig. 1). The scientists conducted an experiment with A. niger, growing on wood covered by a thin layer of nano-TiO2. It took as much as 12 h to stop the growth of the A. niger hyphae, using the UV-A radiation. Even then, the fungus spores remained viable. The long UV-A irradiation period was not able to inactivate the spores. After the source of UV-A radiation had been removed, the germination of spores and the growth of hyphae were noticed. The studies of Yu et al. [189] report that the AOP-based water disinfection was not able, either, to destroy the spores of A. niger. Despite the antifungal capability of the TiO2/UV process, the subsequent hyphae re-growth indicated that the photocatalytic disinfection was not sufficient to completely inactivate A. niger but merely managed to suppress its growth.
In experiments of Sichel et al. [83, 188], the spores of another representative of molds, F. oxysporum, were inactivated not sooner than after 10 h of the TiO2/UV process. Similar results in respect of this species obtained Lonnen et al. [80] as well as Mitoraj et al. [81]. The SEM, TEM, AFM, and XRD examination of A. niger and F. oxysporum cell walls showed that the spores were rugged and wrinkled. There were, however, no traces of nano-TiO2 presence in the spores [112]. Filamentous fungi (particularly their spores) have a fairly high resistance also towards the ZnO/UV process [181, 189, 190]. The underlying factor of the high resistance to photocatalytic processes that molds exhibit is a significant concentration of chitin in their cell wall, up to 15 % of dry matter [186, 187]. This polysaccharide protects directly the plasma membrane, which is very susceptible to the oxidative activity of ROS. A layer of glucans, thinner than in yeasts, covers a relatively thick chitin layer. The glucans are quite resistant to oxidative damages, even though they are slightly more susceptible than chitin. The main compound of the glucans in mold cell wall is β-1,3-glucan, along with a much branched α-1,3-glucan, not present in Saccharomycetaceae. The external layer of the molds cell wall consists of galactoproteins, protein-sugar compounds that constitute around 45 % of cell wall dry matter and exhibit less resistance to oxidative injuries than chitin and glucans [186, 187] (Fig. 7).
Conclusions
Nanotechnology is a relatively young discipline of science. Its rapid development in recent years opens up new opportunities for many areas of human activity. Numerous fields of science, including IT, mechanical engineering, medicine, and many others, are already profiting from its achievements. Nanotechnology may largely contribute towards the fight against many pathogens, thus it may be successfully applied in such areas as food hygiene or public health protection. Infectious agents pose a threat to human health, therefore, an effective disinfection of health-care devices and surfaces appears vital for preventing the pathogens to disseminate. A reduction of infectious agent transmission in the public space can be achieved thanks to the photocatalytic properties of self-disinfecting and self-cleaning surfaces. Their crucial compounds are oxides of some metals, such as TiO2 and ZnO, which, after they have been powdered to NPs, exhibit strong virucidal, bactericidal, and fungicidal properties. The underlying factor hereto is photocatalytic processes induced by the UV radiation. Therefore, metal oxides coatings can become a new, powerful tool in the fight against infectious diseases. The so far commonly applied conventional chemical and pharmaceutical compounds do not provide for such a broad range of application. Nanomaterials, even though a number of them are already in use, are still not sufficiently examined in respect of their entire spectrum of properties, including possible negative side-effects on human health. Thus, the studies on innovative solutions in nanotechnology must continue. As many say, the twenty-first century fight against pathogens is going to be led primarily not by microbiologists but by nanotechnology engineers.
References
Fujishima A, Honda K. Electrochemical photolysis of water at a semiconductor electrode. Nature. 1972;238(5358):37–8.
Benabbou AK, Derriche Z, Felix C, Lejeune P, Guillard C. Photocatalytic inactivation of Escherichia coli—effect of concentration of TiO2 and microorganism, nature, and intensity of UV irradiation. Appl Catal B. 2007;76(3–4):257–63.
Friedmann D, Mendive C, Bahnemann D. TiO2 for water treatment: parameters affecting the kinetics and mechanisms of photocatalysis. Appl Catal B. 2010;99(3–4):398–406.
Matsunaga T, Tomoda R, Nakajima T, Wake H. Photoelectrochemical sterilization of microbial cells by semiconductor powders. FEMS Microbiol Lett. 1985;29(1–2):211–4.
Reddy MP, Venugopal A, Subrahmanyam M. Hydroxyapatite-supported Ag-TiO2 as Escherichia coli disinfection photocatalyst. Water Res. 2007;41(2):379–86.
Jones N, Ray B, Ranjit KT, Manna AC. Antimicrobial activity of ZnO nanoparticles suspensions on a broad spectrum of microorganisms. FEMS Microbiol Lett. 2008;279(1):71–6.
Padmavathy N, Vijayaraghavan R. Enhanced bioactivity of ZnO nanoparticles—an antimicrobial study. Sci Technol Adv Mater. 2008;9:035004.
Yamamoto O. Influence of particle size on the antimicrobial activity of zinc oxide. Int J Inorg Mater. 2001;3(7):643–6.
Zhang I, Ding Y, Povey M, York D. ZnO nanofluids—a potential antibacterial agent. Prog Nat Sci. 2008;18(8):939–44.
Simon-Deckers A, Loo S, Mayne-L’Hermite M, Herlin-Boime N, Menguy N, Reynaud C, et al. Size- composition- and shape-dependent toxicological impact of metal oxide nanoparticles and carbon nanotubes towards bacteria. Environ Sci Technol. 2009;43(21):8423–9.
Allen NS, Edge M, Sandoval G, Verran J, Stratton J, Maltby J. Photocatalytic coatings for environmental applications. Photochem Photobiol. 2005;81(2):279–90.
Costa AL, Ortelli S, Blosi M, Albonetti S, Vaccari A, Dondi M. TiO2 based photocatalytic coatings: from nanostructure to functional properties. Chem Eng J. 2013;225:880–6.
Kambala VS, Naidu R. Disinfection studies on TiO2 thin films prepared by a sol–gel method. J Biomed Nanotechnol. 2009;5(1):121–9.
Carp O, Huisman CL, Reller A. Photoinduced reactivity of titanium dioxide. Prog Solid State Chem. 2004;32(1):33–177.
Cheng CL, Sun DS, Chu WC, Tseng YH, Ho HC, Wang JB, et al. The effects of the bacterial interaction with visible-light responsive titania photocatalyst on the bactericidal performance. J Biomed Sci. 2009;16(1):7.
Hu C, Guo J, Qu J, Hu X. Photocatalytic degradation of pathogenic bacteria with AgI/TiO2 under visible light irradiation. Langmuir. 2007;23(9):4982–7.
Chen F, Yang X, Xu F, Wu Q, Zhang Y. Correlation of photocatalytic bactericidal effect and organic matter degradation of TiO2: part I: observation of phenomena. Environ Sci Technol. 2009;43(4):1180–4.
Jacoby WA, Maness PC, Wolfrum EJ, Blake DM, Fennell JA. Mineralization of bacteria cell mass on a photocatalytic surface in air. Environ Sci Technol. 1998;32(17):2650–3.
Kozlova EA, Safatov AS, Kiselev SA, Marchenko VY, Sergeev AA, Skarnovich MO, et al. Inactivation and mineralization of aerosol deposited model pathogenic microorganisms over TiO2 and Pt/TiO2. Environ Sci Technol. 2010;44(13):5121–6.
Häggström J, Balyozova D, Klabunde KJ, Marchin G. Virucidal properties of metal oxide nanoparticles and their halogen adducts. Nanoscale. 2010;2(4):529–34.
Chung CJ, Lin HI, Tsou HK, Shi ZY, He JL. An antimicrobial TiO2 coating for reducing hospital-acquired infection. J Biomed Mater Res B Appl Biomater. 2008;85(1):220–4.
Lin H, Xu Z, Wang X, Long J, Su W, Fu X, et al. Photocatalytic and antibacterial properties of medical-grade PVC material coated with TiO2 film. J Biomed Mater Res B Appl Biomater. 2008;87(2):425–31.
Akiba N, Hayakawa I, Keh ES, Watanabe A. Antifungal effects of a tissue conditioner coating agent with TiO2 photocatalyst. J Med Dent Sci. 2005;52(4):223–7.
Wolfrum EJ, Huang J, Blake DM, Maness PC, Huang Z, Fiest J, et al. Photocatalytic oxidation of bacteria, bacterial and fungal spores, and model biofilm components to carbon dioxide on titanium dioxide-coated surfaces. Environ Sci Technol. 2002;36(15):3412–9.
Mayer BK, Daugherty E, Abbaszadegan M. Disinfection byproduct formation resulting from settled, filtered, and finished water treated by titanium dioxide photocatalysis. Chemosphere. 2014;117:72–8.
Rizzo L. Inactivation and injury of total coliform bacteria after primary disinfection of drinking water by TiO2 photocatalysis. J Hazard Mater. 2009;165(1–3):48–51.
Sánchez B, Sánchez-Muñoz M, Muñoz-Vicente M, Cobas G, Portela R, Suárez S, et al. Photocatalytic elimination of indoor air biological and chemical pollution in realistic conditions. Chemosphere. 2012;87(6):625–30.
Campoccia D, Montanaro L, Arciola CR. A review of the biomaterials technologies for infection-resistant surfaces. Biomaterials. 2013;34(34):8533–54.
Dasgupta N, Ranjan S, Mundekkad D, Ramalingam C, Shanker R, Kumar A. Nanotechnology in agro-food: from field to plate. Food Res Int. 2015;69:381–400.
Schneider PM. New technologies and trends in sterilization and disinfection. Am J Infect Control. 2013;41(5):S81–6.
Li X, He J. Synthesis of raspberry-like SiO2-TiO2 nanoparticles toward antireflective and self-cleaning coatings. ACS Appl Mater Interfaces. 2013;5(11):5282–90.
Haidaka H, Horikoshi S, Serpone N, Knowland J. In vitro photochemical damage to DNA, RNA and their bases by an inorganic sunscreen agent on exposure to UVA and UVB radiation. J Photochem Photobiol A Chem. 1997;111(1–3):205–13.
Kim S, An YJ. Effect of ZnO and TiO2 nanoparticles preilluminated with UVA and UVB light on Escherichia coli and Bacillus subtilis. Appl Microbiol Biotechnol. 2012;95(1):243–53.
Kühn KP, Chaberny IF, Massholder K, Stickler M, Benz VW, Sonntag HG, et al. Disinfection of surfaces by photocatalytic oxidation with titanium dioxide and UVA light. Chemosphere. 2003;53(1):71–7.
Lee JE, Ko G. Norovirus and MS2 inactivation kinetics of UV-A and UV-B with and without TiO2. Water Res. 2013;47(15):5607–13.
Pablos C, Marugán J, van Grieken R, Serrano E. Emerging micropollutant oxidation during disinfection processes using UV-C, UV-C/H2O2, UV-A/TiO2 and UV-A/TiO2/H2O2. Water Res. 2013;47(3):1237–45.
Robertson JMC, Robertson PKJ, Lawton LA. A comparison of the effectiveness of TiO2 photocatalysis and UVA photolysis for the destruction of three pathogenic microorganisms. J Photochem Photobiol A Chem. 2005;175(1):51–6.
Fujishima A, Rao TN, Tryk DA. Titanium dioxide photocatalysis. J Photochem Photobiol C Photochem Rev. 2000;1(1):1–21.
Mills A, Le Hunte S. An overview of semiconductor photocatalysis. J Photochem Photobiol A Chem. 1997;108(1):1–35.
Linsebigler AL, Lu G, Yates JY. Photocatalysis on TiO2 surfaces: principles, mechanisms, and selected results. Chem Rev. 1995;95(3):735–58.
Li Q, Xie R, Li YW, Mintz EA, Shang JK. Enhanced visible-light-induced photocatalytic disinfection of E. coli by carbon-sensitized nitrogen-doped titanium oxide. Environ Sci Technol. 2007;41(14):5050–6.
Herrmann JM. Heterogeneous photocatalysis: fundamentals and applications to the removal of various types of aqueous pollutants. Catal Today. 1999;53(1):115–29.
Guillard C, Bui TH, Felix C, Moules V, Lina B, Lejeune P. Microbiological disinfection of water and air by photocatalysis. C R Chim. 2008;11(1–2):107–13.
Gerrity D, Ryu H, Crittenden J, Abbaszadegan M. Photocatalytic inactivation of viruses using titanium dioxide nanoparticles and low-pressure UV light. J Environ Sci Health A Tox Hazard Subst Environ Eng. 2008;43(11):1261–70.
Lee JE, Zoh K, Ko G. Inactivation and UV disinfection of murine norovirus with TiO2 under various environmental conditions. Appl Environ Microbiol. 2008;74(7):2111–7.
van der Molen RG, Garssen J, de Klerk A, Claaus FH, Norval M, van Loveren H, et al. Application of a systemic herpes simplex virus type 1 infection in the rat as a tool for sunscreen photoimmunoprotection studies. Photochem Photobiol Sci. 2002;1(8):592–6.
Zan L, Fa W, Peng T, Gong ZH. Photocatalysis effect of nanometer TiO2 and TiO2-coated ceramic plate on Hepatitis B virus. J Photochem Photobiol B. 2007;86(2):165–9.
Sang X, Phan TG, Sugihara S, Yagyu F, Okitsu S, Maneekarn N, et al. Photocatalytic inactivation of diarrheal viruses by visible-light-catalytic titanium dioxide. Clin Lab. 2007;53(7–8):413–21.
Heaselgrave W, Kilvington S. The efficacy of simulated solar disinfection (SODIS) against coxsackievirus, poliovirus and hepatitis A virus. J Water Health. 2012;10(4):531–8.
Cho M, Chung H, Choi W, Yoon J. Different inactivation behaviors of MS-2 phage and Escherichia coli in TiO2 photocatalytic disinfection. Appl Environ Microbiol. 2005;71(1):270–5.
Li Q, Page MA, Mariñas BJ, Shang JK. Treatment of coliphage MS2 with palladium-modified nitrogen-doped titanium oxide photocatalyst illuminated by visible light. Environ Sci Technol. 2008;42(16):6148–53.
Ishiguro H, Nakano R, Yao Y, Kajioka J, Fujishima A, Sunada K, et al. Photocatalytic inactivation of bacteriophages by TiO2-coated glass plates under low-intensity, long-wavelength UV irradiation. Photochem Photobiol Sci. 2011;10(11):1825–9.
Ditta IB, Steele A, Liptrot C, Tobin J, Tyler H, Yates HM, et al. Photocatalytic antimicrobial activity of thin surface films of TiO2, CuO and TiO2/CuO dual layers on Escherichia coli and bacteriophage T4. Appl Microbiol Biotechnol. 2008;79(1):127–33.
Han W, Zhang Z, Cao W, Yang D, Shigeharu T, Yoshio O, et al. The inactivation effect of photocatalytic titanium apatie filter on SARS virus. Prog Biochem Biophys. 2004;11:982–5.
Nakano R, Ishiguro H, Yao Y, Kajioka J, Fujishima A, Sunada K, et al. Photocatalytic inactivation of influenza virus by titanium dioxide thin film. Photochem Photobiol Sci. 2012;11(8):1293–8.
Cui H, Jiang J, Gu W, Sun C, Wu D, Yang T, et al. Photocatalytic inactivation efficiency of anatase nano-TiO2 sol on the H9N2 avian influenza virus. Photochem Photobiol. 2010;86(5):1135–9.
Josset S, Taranto J, Keller N, Keller V, Lett MC. Photocatalytic treatment of bioaerosols: impact of the reactor design. Environ Sci Technol. 2010;44(7):2605–11.
Zhao Y, Aarnink AJ, Xin H. Inactivation of airborne Enterococcus faecalis and infectious bursal disease virus using a pilot-scale ultraviolet photocatalytic oxidation scrubber. J Air Waste Manag Assoc. 2014;64(1):38–46.
Xu R, Liu X, Zhang P, Ma H, Liu G, Xia Z. The photodestruction of virus in nano-TiO2 suspension. J Wuhan Univ Technol. 2007;22(3):422–5.
Kashige N, Kakita Y, Nakashima Y, Miake F, Watanabe K. Mechanism of the photocatalytic inactivation of Lactobacillus casei phage PL-1 by titania thin film. Curr Microbiol. 2001;42(3):184–9.
Kim JY, Lee C, Cho M, Yoon J. Enhanced inactivation of E. coli and MS-2 phage by silver ions combined with UV-A and visible light irradiation. Water Res. 2008;42(1–2):356–62.
Sjogren JC, Sierka RA. Inactivation of phage MS2 by iron-aided titanium dioxide photocatalysis. Appl Environ Microbiol. 1994;60(1):344–7.
Liga MV, Bryant EL, Colvin VL, Li Q. Virus inactivation by silver doped titanium dioxide nanoparticles for drinking water treatment. Water Res. 2011;45(2):535–44.
Liga MV, Maguire-Boyle SJ, Jafry HR, Barron AR, Li Q. Silica decorated TiO2 for virus inactivation in drinking water-simple synthesis method and mechanisms of enhanced inactivation kinetics. Environ Sci Technol. 2013;47(12):6463–70.
Nakano R, Hara M, Ishiguro H, Yao Y, Ochiai T, Nakata K, et al. Broad spectrum microbicidal activity of photocatalysis by TiO2. Catalysts. 2013;3(1):310–23.
Paspaltsis I, Berberidou C, Poulios I, Sklaviadis T. Photocatalytic degradation of prions using the photo-Fenton reagent. J Hosp Infect. 2009;71(2):149–56.
Paspaltsis I, Kotta K, Lagoudaki R, Grigoriadis N, Poulios I, Sklaviadis T. Titanium dioxide photocatalytic inactivation of prions. J Gen Virol. 2006;87(10):3125–30.
Bassetti M, Merelli M, Temperoni C, Astilean A. New antibiotics for bad bugs: where are we? Ann Clin Microbiol Antimicrob. 2013;12:22.
Yang YS, Lee YT, Tsai WC, Kuo SC, Sun JR, Yang CH, et al. Comparison between bacteremia caused by carbapenem resistant Acinetobacter baumannii and Acinetobacter nosocomialis. BMC Infect Dis. 2013;13:311.
Correa L, Martino MD, Siqueira I, Pasternak J, Gales AC, Silva CV, et al. A hospital-based matched case–control study to identify clinical outcome and risk factors associated with carbapenem-resistant Klebsiella pneumoniae infection. BMC Infect Dis. 2013;13:80.
Mohanty S, Maurya V, Gaind R, Deb M. Phenotypic characterization and colistin susceptibilities of carbapenem-resistant of Pseudomonas aeruginosa and Acinetobacter spp. J Infect Dev Ctries. 2013;7(11):880–7.
Yahdi M, Abdelmageed S, Lowden J, Tannenbaum L. Vancomycin-resistant enterococci colonization-infection model: parameter impacts and outbreak risks. J Biol Dyn. 2012;6(2):645–62.
Singer J, Merz A, Frommelt L, Fink B. High rate of infection control with one-stage revision of septic knee prostheses excluding MRSA and MRSE. Clin Orthop Relat Res. 2012;470(5):1461–71.
Tiwari HK, Sen MR. Emergence of vancomycin resistant Staphylococcus aureus (VRSA) from a tertiary care hospital from northern part of India. BMC Infect Dis. 2006;6:156.
Gouveia EL, Reis JN, Flannery B, Cordeiro SM, Lima JB, Pinheiro RM, et al. Clinical outcome of pneumococcal meningitis during the emergence of pencillin-resistant Streptococcus pneumoniae: an observational study. BMC Infect Dis. 2011;11:323.
Aboelzahab A, Azad AM, Dolan S, Goel V. Mitigation of Staphylococcus aureus-mediated surgical site infections with photoactivated TiO2 coatings on Ti implants. Adv Healthc Mater. 2012;1(3):285–91.
Kim B, Kim D, Cho D, Cho S. Bactericidal effect of TiO2 photocatalyst on selected food-borne pathogenic bacteria. Chemosphere. 2003;52(1):277–81.
Azam A, Ahmed AS, Oves M, Khan MS, Habib SS, Memic A. Antimicrobial activity of metal oxide nanoparticles against gram-positive and gram-negative bacteria: a comparative study. Int J Nanomedicine. 2012;7:6003–9.
Azimzadehirani M, Elahifard M, Haghighi S, Gholami M. Highly efficient hydroxyapatite/TiO2 composites covered by silver halides as E. coli disinfectant under visible light and dark media. Photochem Photobiol Sci. 2013;12(10):1787–94.
Lonnen J, Kilvington LJ, Kehoe SC, Al-Toutai F, McGuigan KG. Solar and photocatalytic disinfection of protozoan, fungal and bacterial microbes in drinking water. Water Res. 2005;39(5):877–83.
Mitoraj D, Jańczyk A, Strus M, Kisch H, Stochel G, Heczko PB, et al. Visible light inactivation of bacteria and fungi by modified titanium dioxide. Photochem Photobiol Sci. 2007;6(6):642–8.
Seven O, Dindar B, Aydemir S, Metin D, Ozinel A, Icli S. Solar photocatalytic disinfection of a group of bacteria and fungi aqueous suspensions with TiO2, ZnO and Sahara desert dust. J Photochem Photobiol A Chem. 2004;165(1–3):103–7.
Sichel C, Tello J, de Cara M, Fernãndez-Ibáñez P. Effect of UV solar intensity and dose on the photocatalytic disinfection of bacteria and fungi. Catal Today. 2007;129(1–2):152–60.
Li B, Logan BE. The impact of ultraviolet light on bacterial adhesion to glass and metal oxide-coated surface. Colloids Surf B Biointerfaces. 2005;41(2–3):153–61.
Maness PC, Smolinski S, Blake DM, Huang Z, Wolfrum EJ, Jacoby WA. Bactericidal activity of photocatalytic TiO2 reaction: toward an understanding of its killing mechanism. Appl Environ Microbiol. 1999;65(9):4094–8.
Tong T, Binh CT, Kelly JJ, Gaillard JF, Gray KA. Cytotoxicity of commercial nano-TiO2 to Escherichia coli assessed by high-throughput screening: effects of environmental factors. Water Res. 2013;47(7):2352–62.
Foster HA, Ditta IB, Varghese S, Steele A. Photocatalytic disinfection using titanium dioxide: spectrum and mechanism of antimicrobial activity. Appl Microbiol Biotechnol. 2011;90(6):1847–68.
Tsunag YH, Sun JS, Huang YC, Lu CH, Chang WH, Wang CC. Studies of photokilling of bacteria using titanium dioxide nanoparticles. Artif Organs. 2008;32(2):167–74.
Ferin J, Oberdörster G. Biological effects and toxicity assessment of titanium dioxides: anatase and rutile. Am Ind Hyg Assoc J. 1985;46(2):69–72.
Hwang YK, Park SS, Lim JH, Won YS, Huh S. Preparation of anatase/rutile mixed-phase titania nanoparticles for dye-sensitized solar cells. J Nanosci Nanotechnol. 2013;13(3):2255–61.
Huang Z, Maness PC, Blake DM, Wolfrum EJ, Smolinski SL, Jacoby WA. Bactericidal mode of titanium dioxide photocatalysis. J Photochem Phytobiol A Chem. 2000;130(2–3):163–70.
Joost U, Juganson K, Visnapuu M, Mortimer M, Kahru A, Nõmmiste E, et al. Photocatalytic antibacterial activity of nano-TiO2 (anatase)-based thin films: effects on Escherichia coli cells and fatty acids. J Photochem Photobiol B. 2015;142:178–85.
Liou JW, Chang HH. Bactericidal effects and mechanisms of visible light-responsive titanium dioxide photocatalysts on pathogenic bacteria. Arch Immunol Ther Exp (Warsz). 2012;60(4):267–75.
Pigeot-Rémy S, Simonet F, Atlan D, Lazzaroni JC, Guillard C. Bactericidal efficiency and mode of action: a comparative study of photochemistry and photocatalysis. Water Res. 2012;46(10):3208–18.
Salih FM, Pillay AE. Efficiency of solar water disinfection photocatalized by titanium dioxide of varying particle size. J Water Health. 2007;5(3):335–40.
Horie Y, David DA, Taya M, Tone S. Effects of light intensity and titanium dioxide concentration on photocatalytic sterilization rates of microbial cells. Ind Eng Chem Res. 1996;35(11):3920–6.
Rincón AG, Pulgarin C. Photocatalytic inactivation of E. coli: effect of (continuous-intermittent) light intensity and of (suspended-fixed) TiO2 concentration. Appl Catal B. 2003;44(3):263–84.
Ireland JC, Klostermann P, Rice EW, Clark RM. Inactivation of Escherichia coli by titanium dioxide photocatalytic oxidation. Appl Environ Microbiol. 1993;59(5):1668–70.
Egerton TA, Kosa SA, Christensen PA. Photoelectrocatalytic disinfection of E. coli suspensions by iron doped TiO2. Phys Chem Chem Phys. 2006;8(3):398–406.
Reeves JF, Davies SJ, Dodd NJF, Jha AN. Hydroxyl radicals (*OH) are associated with titanium dioxide (TiO2) nanoparticle-induced cytotoxicity and oxidative DNA damage in fish cells. Mutat Res. 2008;640(1–2):113–22.
Cho M, Chung H, Choi W, Yoon J. Linear correlation between inactivation of E. coli and OH radical concentration in TiO2 photocatalytic disinfection. Water Res. 2004;38(4):1069–77.
Bekbölet M, Araz CV. Inactivation of Escherichia coli by photocatalytic oxidation. Chemosphere. 1996;32(5):959–65.
Salih FM. Enhancement of solar inactivation of Escherichia coli by titanium dioxide photocatalytic oxidation. J Appl Microbiol. 2002;92(5):920–6.
Kim S, Ghafoor K, Lee J, Feng M, Hong J, Lee DU, et al. Bacterial inactivation in water, DNA strand breaking, and membrane damage induced by ultraviolet-assisted titanium dioxide photocatalysis. Water Res. 2013;47(13):4403–11.
Liu P, Duan W, Wang Q, Li X. The damage of outer membrane of Escherichia coli in the presence of TiO2 combined with UV light. Colloids Surf B Biointerfaces. 2010;78(2):171–6.
Hirakawa K, Mori M, Yoshida M, Oikawa S, Kawanishi S. Photo-irradiated titanium dioxide catalyzes site specific DNA damage via generation of hydrogen peroxide. Free Radic Res. 2004;38(5):439–47.
Lanao M, Ormad MP, Goñi P, Miguel N, Mosteo R, Ovelleiro JL. Inactivation of Clostridium perfringens spores and vegetative cells by photolysis and TiO2 photocatalysis with H2O2. Solar Energy. 2010;84(4):703–9.
Kiwi J, Nadtochenko V. New evidence for TiO2 photocatalysis during bilayer lipid peroxidation. J Phys Chem B. 2004;108(45):17657–84.
Bacsa R, Kiwi J, Ohno T, Albers P, Nadtochenko V. Preparation, testing and characterization of doped TiO2 active in the peroxidation of biomolecules under visible light. J Phys Chem B. 2005;109(12):5994–6003.
Kiwi J, Nadtochenko V. Evidence for the mechanism of photocatalytic degradation of the bacterial wall membrane at the TiO2 interface by ATR-FTIR and laser kinetic spectroscopy. Langmuir. 2005;21(10):4631–41.
Amézaga-Madrid P, Silveyra-Morales R, Córdoba-Fierro L, Nevárez-Moorillón GV, Miki-Yoshida M, Orrantia-Borunda E, et al. TEM evidence of ultrastructural alteration on Pseudomonas aeruginosa by photocatalytic TiO2 thin films. J Photochem Photobiol B. 2003;70(1):45–50.
Banerjee S, Gopal J, Muraleedharan P, Tyagi AK, Raj B. Physics and chemistry of photocatalytic titanium dioxide: visualization of bactericidal activity using atomic force microscopy. Curr Sci. 2006;90(10):1378–83.
Nadtochenko VA, Rincon AG, Stanca SE, Kiwi J. Dynamics of E. coli membrane cell peroxidation during TiO2 photocatalysis studied by ATR-FTIR spectroscopy and AFM microscopy. J Photochem Photobiol A. 2005;169(2):131–7.
Vacaroiu C, Enache M, Gartner M, Popescu G, Anastasescu M, Brezeanu A, et al. The effect of thermal treatment on antibacterial properties of nanostructured TiO2 (N) films illuminated with visible light. World J Microbiol Biotechnol. 2009;25(1):27–31.
Dalrymple OK, Stefanakos E, Trotz MA, Goswami DY. A review of the mechanisms and modeling of photocatalytic disinfection. Appl Catal B. 2010;98(1–2):27–38.
Gogniat G, Dukan S. TiO2 photocatalysis causes DNA damage via Fenton reaction-generated hydroxyl radicals during the recovery period. Appl Environ Microbiol. 2007;73(23):7740–3.
Wamer WG, Yin JJ, Wei RR. Oxidative damage to nucleic acids photosensitized by titanium dioxide. Free Radic Biol Med. 1997;23(6):851–8.
Ashikaga T, Wada M, Kobayashi H, Mori M, Katsumura Y, Fukui H, et al. Effect of the photocatalytic activity of TiO2 on plasmid DNA. Mutat Res. 2000;466(1):1–7.
Gao M, An T, Li G, Nie X, Yip HY, Zhao H, et al. Genetic studies of the role of fatty acid and coenzyme A in photocatalytic inactivation of Escherichia coli. Water Res. 2012;46(13):3951–7.
Imlay JA, Chin SM, Linn S. Toxic DNA damage by hydrogen peroxide through the Fenton reaction in vivo and in vitro. Science. 1988;240(4852):640–2.
Ndounla J, Spuhler D, Kenfack S, Wéthé J, Pulgarin C. Inactivation by solar photo-Fenton in pet bottles of wild enteric bacteria of natural well water: absence of re-growth after one week of subsequent storage. Appl Catal B. 2013;129:309–17.
Dukan S, Nyström T. Oxidative stress defense and deterioration of growth-arrested Escherichia coli cells. J Biol Chem. 1999;274(37):26027–32.
Kim YG. Collaborative effects of Photobacterium CuZn superoxide dismutase (SODs) and human AP endonuclease in DNA repair and SOD-deficient Escherichia coli under oxidative stress. Free Radic Biol Med. 2004;36(2):173–9.
Kim SY, Nishioka M, Taya M. Promoted proliferation of an SOD-deficient mutant of Escherichia coli under oxidative stress induced by photoexcited TiO2. FEMS Microbiol Lett. 2004;236(1):109–14.
Ojima Y, Nishioka M, Taya M. Metabolic alternations in SOD-deficient Escherichia coli cells when cultivated under oxidative stress from photoexcited titanium dioxide. Biotechnol Lett. 2008;30(6):1107–13.
Sunada K, Watanabe T, Hashimoto K. Studies on photokilling of bacteria on TiO2 thin film. J Photochem Photobiol A. 2003;156(1–3):227–33.
Berney M, Weilenmann HU, Simonetti A, Egli T. Efficacy of solar disinfection of Escherichia coli, Shigella flexneri, Salmonella Typhimurium and Vibrio cholerae. J Appl Microbiol. 2006;101(4):828–36.
Nitzan Y, Ashkenazi H. Photoinactivation of Acinetobacter baumannii and Escherichia coli by a cationic hydrophilic porphyrin at various light wavelengths. Curr Microbiol. 2001;42(6):408–14.
Gupta K, Singh RP, Pandey A, Pandey A. Photocatalytic antibacterial performance of TiO2 and Ag-doped TiO2 against S. aureus, P. aeruginosa and E. coli. Beilstein J Nanotechnol. 2013;4:345–51.
Liu HL, Yang TCK. Photocatalityc inactivation of Escherichia coli and Lactobacillus helveticus by ZnO and TiO2 activated with ultraviolet light. Process Biochem. 2003;39(4):475–81.
Planchon M, Ferrari R, Guyot F, Gélabert A, Menguy N, Chanéac C, et al. Interaction between Escherichia coli and TiO2 nanoparticles in natural and artificial waters. Colloids Sur, B Biointerfaces. 2013;102:158–64.
Pathakoti K, Morrow S, Han C, Pelaez M, He X, Dionysiou DD, et al. Photoinactivation of Escherichia coli by sulfur-doped and nitrogen-fluorine-codoped TiO2 nanoparticles under solar simulated light and visible light irradiation. Environ Sci Technol. 2013;47(17):9988–96.
Rizzo L, Della Sala A, Fiorentino A, Li Puma G. Disinfection of urban wastewater by solar driven and UV lamp—TiO2 photocatalysis: effect on a multi drug resistant Escherichia coli strain. Water Res. 2014;53:145–52.
Cho M, Cates EL, Kim JH. Inactivation and surface interactions of MS-2 bacteriophage in a TiO2 photoelectrocatalytic reactor. Water Res. 2011;45(5):2104–10.
Szczawiński J, Tomaszewski H, Jackowska-Tracz A, Szczawińska ME. Effect of UV radiation on survival of Salmonella Enteritidis on the surface of ceramic tiles coated with TiO2. Bull Vet Inst Pulawy. 2010;54:479–83.
Wong MS, Chu WC, Sun DS, Huang HS, Chen JH, Tsai PJ, et al. Visible-light-induced bactericidal activity of a nitrogen-doped titanium photocatalyst against human pathogens. Appl Environ Microbiol. 2006;72(9):6111–6.
Cheng YW, Chan RCY, Wong PK. Disinfection of Legionella pneumophila by photocatalytic oxidation. Water Res. 2007;41(4):842–52.
Danshvar D, Niaei A, Akbari S, Aber S, Kazemian N. Photocatalytic disinfection of water polluted by Pseudomonas aeruginosa. Global Nest J. 2007;9(3):1–5.
Upritchard HG, Yang J, Bremer PJ, Lamont IL, McQuillan AJ. Adsorption to metal oxides of the Pseudomonas aeruginosa siderophore pyoverdine and implications for bacterial biofilm formation on metals. Langmuir. 2007;23(13):7189–95.
Bonetta S, Bonetta S, Motta F, Strini A, Carraro E. Photocatalytic bacterial inactivation by TiO2-coated surfaces. AMB Express. 2013;3(1):59.
Armon R, Weltch-Cohen G, Bettane P. Disinfection of Bacillus spp. spores in drinking water by TiO2 photocatalysis as a model for Bacillus anthracis. Water Sci Technol. 2004;4(2):7–14.
Kau JH, Sun DS, Huang HH, Wong MS, Lin HC, Chang HH. Role of visible light-activated photocatalyst on the reduction of anthrax spore-induced mortality in mice. PLoS One. 2009;4(1), e4167.
Prasad GK, Agarval GS, Sigh B, Rai GP, Vijayaraghavan R. Photocatalytic inactivation of Bacillus anthracis by titaniana nomaterials. J Hazard Mater. 2009;165(1–3):506–10.
Nhung TT, Nagata H, Takahashi A, Aihara M, Okamoto T, Shimohata T, et al. Sterilization effect of UV light on Bacillus spores using TiO2 films depends on wavelength. J Med Invest. 2012;59(1–2):53–8.
Zhao J, Krishna V, Hua B, Moudgil B, Koopman B. Effect of UVA irradiance on photocatalytic and UVA inactivation of Bacillus cereus spores. J Photochem Photobiol B. 2009;94(2):96–100.
Pham HN, McDowell T, Wilkins E. Photocatalytically-mediated disinfection of water using TiO2 as a catalyst and spore-forming Bacillus pumilis as a model. J Environ Sci Health A Environ Sci Eng Toxic Hazard Subst Control. 1995;30(3):627–36.
Shah AG, Shetty PC, Ramachandra CS, Bhat NS, Laxmikanth SM. In vitro assessment of photocatalytic titanium oxide surface modified stainless steel orthodontic brackets for antiadherent and antibacterial properties against Lactobacillus acidophilus. Angle Orthod. 2011;81(6):1028–35.
Dunlop PSM, McMurray TA, Hamilton JWJ, Byrne JA. Photocatalytic inactivation of Clostridium perfringens spores on TiO2 electrodes. J Photochem Photobiol A Chem. 2008;196(1):113–9.
Venieri D, Chatzisymeon E, Gonzalo MS, Rosal R, Mantzavinos D. Inactivation of Enterococcus faecalis by TiO2-mediated UV and solar irradiation in water and wastewater: culture techniques never say the whole truth. Photochem Photobiol Sci. 2011;10(11):1744–50.
Ammendolia MG, Iosi F, De Berardis B, Guccione G, Superti F, Conte MP, et al. Listeria monocytogenes behaviour in presence of non-UV-irradiated titanium dioxide nanoparticles. PLoS One. 2014;9(1), e84986.
Long M, Wang J, Zhuang H, Zhang Y, Wu H, Zhang J. Performance and mechanism of standard nano-TiO2 (P-25) in photocatalytic disinfection of foodborne microorganisms—Salmonella Typhimurium and Listeria monocytogenes. Food Control. 2014;39:68–74.
Markowska-Szczupak A, Ulfig K, Morawski AW. The application of titanium dioxide for deactivation of bioparticulates: an overview. Catal Today. 2011;169(1):249–57.
Hitkova H, Stoyanova A, Ivanova N, Sredkova M, Popova V, Iordanova R, et al. Study of antibacterial activity of nonhydrolytic synthesized TiO2 against E. coli, P. aeruginosa and S. aureus. J Optoelectron Biomed Mater. 2012;4(1):9–17.
Chung CJ, Lin HI, Chou CM, Hsieh PY, Hsiao CH, Shi ZY, et al. Inactivation of Staphylococcus aureus and Escherichia coli under various light sources on photocatalytic titanium dioxide thin film. Surf Coat Technol. 2009;203(8):1081–5.
Li Y, Ma M, Wang X. Inactivated properties of activated carbon-supported TiO2 nanoparticles for bacteria and kinetic study. J Environ Sci. 2008;20(12):1527–33.
Malato S, Blanco J, Alarcón DC, Maldonaldo MI, Fernández-Ibáñez P, Gernjak W. Photocatalytic decontamination and disinfection of water with solar collectors. Catal Today. 2007;122(1–2):137–49.
Muszkat L, Feigelson L, Bir L, Muszkat KA, Teitel M, Dornay I, et al. Solar photo-inactivation of phytophatogenes by trace level hydrogen peroxide and titanium dioxide photocatalysis. Phytoparasitica. 2005;33(3):267–74.
Pal A, Pehkonen SO, Yu LE, Ray MB. Photocatalytic inactivation of Gram-positive and Gram-negative bacteria using fluorescent light. J Photochem Photobiol A. 2007;186(2–3):335–41.
Rincón AG, Pulgarin C. Use of coaxial photocatalytic reactor (caphore) in the TiO2 photo-assisted treatment of mixed E. coli and Bacillus spp. and bacterial community present in wastewater. Catal Today. 2005;101(3–4):331–44.
Skorb EV, Antonouskaya LI, Belyasova NA, Shchukin DG, Möhwald H, Sviridov DV. Antibacterial activity of thin-film photocatalysts based on metal-modified TiO2 and TiO2:In2O3 nanocomposite. Appl Catal B. 2008;84(1–2):94–9.
Desai VS, Kowshik M. Antimicrobial activity of titanium dioxide nanoparticles synthesized by sol–gel technique. Res J Microbiol. 2009;4(3):97–103.
Dunlop PSM, Sheeran CP, Byrne JA, McMahon MAS, Boyle MA, McGuigan KG. Inactivation of clinically relevant pathogens by photocatalytic coatings. J Photochem Photobiol A. 2010;216(2–3):303–10.
Kangwansupamonkon W, Lauruengtana V, Surassmo S, Ruktanonchai U. Antibacterial effect of apatite-coated titanium dioxide for textiles applications. Nanomedicine. 2009;5(2):240–9.
Kubacka A, Ferrer M, Martínez-Arias A, Fernández-García M. Ag promotion of TiO2-anatase disinfection capability: study of Escherichia coli inactivation. Appl Catal B. 2008;84(1–2):87–93.
Pelgrift RY, Friedman AJ. Nanotechnology as a therapeutic tool to combat microbial resistance. Adv Drug Deliv Rev. 2013;65(13–14):1803–15.
Necula BS, Fratila-Apachitei LE, Zaat SA, Apachitei I, Duszczyk J. In vitro antibacterial activity of porous TiO2-Ag composite layers against methicillin-resistant Staphylococcus aureus. Acta Biomater. 2009;5(9):3573–80.
Ibáñez JA, Litter MI, Pizarro RA. Photocatalytic bactericidal effect of TiO2 on Enterobacter cloacae: comparative study with other gram (−) bacteria. J Photochem Photobiol A Chem. 2003;157(1):81–5.
Gordon T, Perlstein B, Houbara O, Felner I, Banin E, Margel S. Synthesis and characterization of zinc/iron oxide composite nanoparticles and their antibacterial properties. Colloids Surf A Physicochem Eng Asp. 2011;374(1–3):1–8.
Luo Z, Wu Q, Xue J, Ding Y. Selectively enhanced antibacterial effects and ultraviolet activation of antibiotics with ZnO nanorods against Escherichia coli. J Biomed Nanotechnol. 2013;9(1):69–76.
Tankhiwale R, Bajpai SK. Preparation, characterization and antibacterial applications of ZnO-nanoparticles coated polyethylene films for food packaging. Colloids Surf B Biointerfaces. 2012;90:16–20.
Jin T, Sun D, Su JY, Zhang H, Sue HJ. Antimicrobial efficacy of zinc oxide quantum dots against Listeria monocytogenes, Salmonella Enteritidis, and Escherichia coli O157:H7. J Food Sci. 2009;74(1):M46–52.
Raghupathi KR, Koodali RT, Manna AC. Size-dependent bacterial growth inhibition and mechanism of antibacterial activity of zinc oxide nanoparticles. Langmuir. 2011;27(7):4020–8.
Siddique S, Shah ZH, Shahid S, Yasmin F. Preparation, characterization and antibacterial activity of ZnO nanoparticles on broad spectrum of microorganisms. Acta Chim Slov. 2013;60(3):660–5.
Xie Y, He Y, Irwin PL, Jin T, Shi X. Antibacterial activity and mechanism of action of zinc oxide nanoparticles against Campylobacter jejuni. Appl Environ Microbiol. 2011;77(7):2325–31.
Jain A, Bhargava R, Poddar P. Probing interaction of gram-positive and gram-negative bacterial cells with ZnO nanorods. Mater Sci Eng C Mater Biol Appl. 2013;33(3):1247–53.
Takeda M, Saijo Y, Yuasa M, Kanazawa A, Araki A, Kishi R. Relationship between sick building syndrome and indoor environmental factors in newly built Japanese dwellings. Int Arch Occup Environ Health. 2009;82(5):583–93.
Thabet S, Simonet F, Lemaire M, Guillard C, Cotton P. Impact of photocatalysis on fungal cells: depiction of cellular and molecular effects on Saccharomyces cerevisiae. Appl Environ Microbiol. 2014;80(24):7527–35.
Perelshtein I, Applerot G, Perkas N, Grinblat J, Gedanken A. A one-step process for the antimicrobial finishing of textiles with crystalline TiO2 nanoparticles. Chem Eur J. 2012;18(15):4575–82.
Xiao G, Zhang X, Zhao Y, Su H, Tan T. The behavior of active bactericidal and antifungal coating under visible light irradiation. Appl Surf Sci. 2014;292:756–63.
Dizaj SM, Lotfipour F, Barzegar-Jalali M, Zarrintan MH, Adibkia K. Antimicrobial activity of the metals and metal oxide nanoparticles. Mater Sci Eng C Mater Biol Appl. 2014;44:278–84.
Gondal MA, Alzahrani AJ, Randhawa MA, Siddiqui MN. Morphology and antifungal effect of nano-ZnO and nano-Pd-doped nano-ZnO against Aspergillus and Candida. J Environ Sci Healtht A Tox Hazard Subst Environ Eng. 2012;47(10):1413–8.
Kairyte K, Kadys A, Luksiene Z. Antibacterial and antifungal activity of photoactivated ZnO nanoparticles in suspension. J Photochem Photobiol B. 2013;128:78–84.
Sharma D, Rajput J, Kaith BS, Kaur M, Sharma S. Synthesis of ZnO nanoparticles and study of their antibacterial and antifungal properties. Thin Solid Films. 2010;519(3):1224–9.
Lipovsky A, Nitzan Y, Gedanken A, Lubart R. Antifungal activity of ZnO nanoparticles—the role of ROS mediated cell injury. Nanotechnology. 2011;22(10):105101.
Aguilar-Uscanga B, François JM. A study of the yeast cell wall composition and structure in response to growth conditions and mode of cultivation. Lett Appl Microbiol. 2003;37(3):268–74.
Barreto-Bergter E, Figueiredo RT. Fungal glycans and the innate immune recognition. Front Cell Infect Microbiol. 2014;4:145.
Cassone A, Marconi P, Bistoni F. Cell wall of Candida albicans and host response. Crit Rev Microbiol. 1987;5(1):87–95.
Sichel C, de Cara M, Tello J, Blanco J, Fernández-Ibáñez P. Solar photocatalytic disinfection of agricultural pathogenic fungi: Fusarium species. Appl Catal B. 2007;74(1–2):152–60.
Yu KP, Huang YT, Yang SC. The antifungal efficacy of nano-metals supported TiO2 and ozone on the resistant Aspergillus niger spore. J Hazard Mater. 2013;261:155–62.
He L, Liu Y, Mustapha A, Lin M. Antifungal activity of zinc oxide nanoparticles against Botrytis cinerea and Penicillium expansum. Microbiol Res. 2011;166(3):207–15.
Ye SY, Fan ML, Song XL, Luo SC. Enhanced photocatalytic disinfection of P. expansum in cold storage using a TiO2/ACF film. Int J Food Microbiol. 2010;136(3):332–9.
Chen F, Yang X, Wu Q. Antifungal capability of TiO2 coated film on moist wood. Build Environ. 2009;44(5):1088–93.
Author information
Authors and Affiliations
Corresponding author
Additional information
Competing Interests
The authors declare that they have no competing interests.
Authors’ Contributions
JB performed the overall review and drafted the manuscript. JZ conducted the research work on the latest developments in the application of the TiO2/UV and ZnO/UV photocatalysis in viruses, prions, bacteria, yeasts, and molds eradication and helped draft the manuscript and sequence alignment. JPC is the main coordinator of this manuscript and prepared its revision. All authors read and approved the final manuscript.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0), which permits use, duplication, adaptation, distribution, and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Bogdan, J., Zarzyńska, J. & Pławińska-Czarnak, J. Comparison of Infectious Agents Susceptibility to Photocatalytic Effects of Nanosized Titanium and Zinc Oxides: A Practical Approach. Nanoscale Res Lett 10, 309 (2015). https://doi.org/10.1186/s11671-015-1023-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s11671-015-1023-z


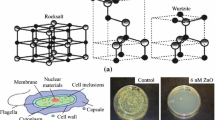



 ) of layers encircling the nucleic acid in non-enveloped (a) and enveloped (b) viruses to damages induced by hydroxyl radicals (•OH). Susceptibility of the various layers encircling the viral nucleic acid to oxidative damages is almost identical (plasma membrane ≈ tegument ≈ capsid)
) of layers encircling the nucleic acid in non-enveloped (a) and enveloped (b) viruses to damages induced by hydroxyl radicals (•OH). Susceptibility of the various layers encircling the viral nucleic acid to oxidative damages is almost identical (plasma membrane ≈ tegument ≈ capsid)



 ) of yeasts cell envelope compounds to damages induced by hydroxyl radicals (•OH). Susceptibility of the various compounds of the yeasts cell envelope (cell wall and plasma membrane) to oxidative damages presents the following order: phospholipids > glycoproteins > glucans > chitin
) of yeasts cell envelope compounds to damages induced by hydroxyl radicals (•OH). Susceptibility of the various compounds of the yeasts cell envelope (cell wall and plasma membrane) to oxidative damages presents the following order: phospholipids > glycoproteins > glucans > chitin
 ) of molds cell envelope compounds to damages induced by hydroxyl radicals (•OH). Susceptibility of the various compounds of the molds cell envelope (cell wall and plasma membrane) to oxidative damages presents the following order: phospholipids > glycoproteins > glucans > chitin
) of molds cell envelope compounds to damages induced by hydroxyl radicals (•OH). Susceptibility of the various compounds of the molds cell envelope (cell wall and plasma membrane) to oxidative damages presents the following order: phospholipids > glycoproteins > glucans > chitin